Perfectus Biomed Group have an actively innovative culture, and we strive to practice science that improves lives. Our unique specialism in biofilms, and our experience in customisable tissue models built the base for this particularly interesting study.
Biofilm forming bacteria can adhere to and then colonize acute and chronic wounds. The efficacy of antibiotic therapy treatments may be decreased by the presence of biofilms and multidrug-resistant (MDR) bacteria. The Centre for Disease Control and Prevention estimate that 65% of all human infectious diseases are caused by bacteria-containing biofilms, while the National Institutes of Health estimate that the true percentage is closer to 80%. There are over 14 million biofilm infections per year and over 350,000 biofilm-related deaths. Given the preponderance of biofilms in wounds and the associated impact on public health, it is important to explore anti-biofilm therapeutics that can prevent formation and persistence of biofilm in acute wounds, consequently decreasing the incidence of chronic wounds and improving wound-healing recovery times.
Perfectus Biomed have created customisable ex vivo wounded skin models that can be used to assess the efficacy of antimicrobial and wound-healing therapies. These models bridge the gap between in vitro and in vivo studies and have certain advantages over both study types. Ex vivo models are more predictive of clinical success compared to in vitro experiments, while remaining more cost effective and an alternative to live animal testing. Ex vivo models enable evaluations of the anti-biofilm efficacy and cytotoxicity of therapeutic formulations, dressings, and devices. They may also be used to investigate immune response and wound closure.
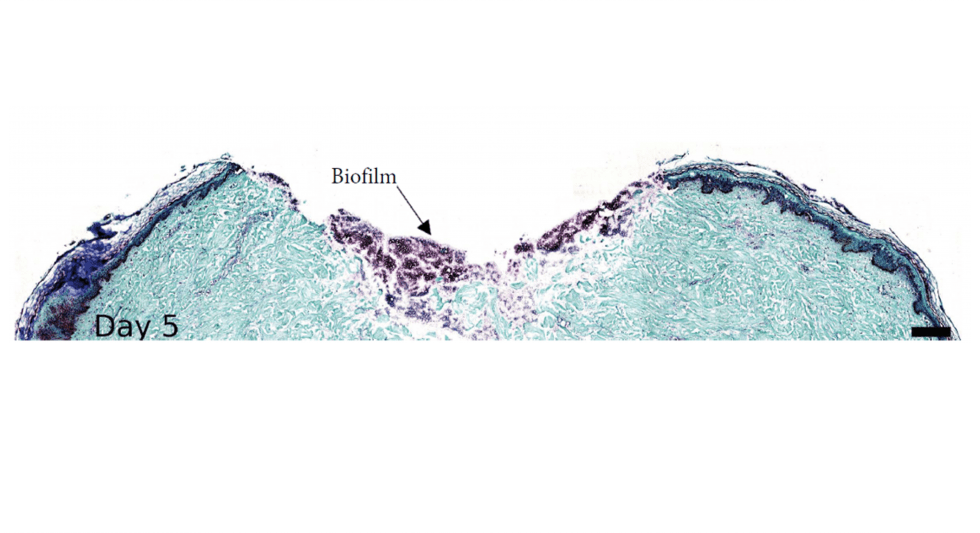
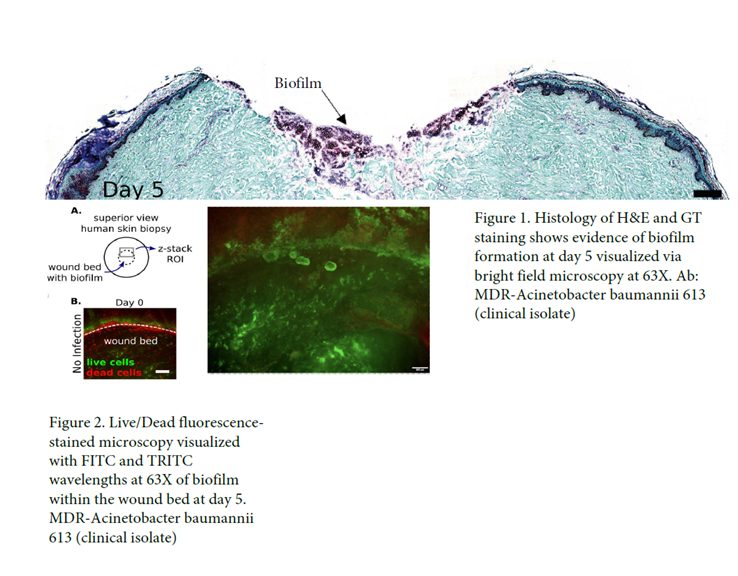
Our team in the US used this model to establish biofilm formulations of multidrug resistant organisms. Wounded explants were infected, and bacteria were allowed to form a biofilm for 7 days. Each day explants were collected and analysed to quantify the amount of planktonic and adherent bacteria. They concluded that using this model had proven antiseptic efficacy against biofilm wound infections with reproducibility.
Our novel ex vivo tissue models are a key testing resource to prove the antimicrobial efficacy of chronic wound care products and devices. The model offers a more cost effective and accelerated alternative to live animal testing. Contact us today to discuss how we can provide outsourced customisable testing to support your products research and development.